If you have ever suffered from vertigo, you will be familiar with that dreadful sensation of feeling off-balance and dizzy, as if you are spinning, or the world around you is spinning.
Vertigo is a symptom, not a disorder in itself or a diagnosis, explains vestibular physiotherapist Sheila Barrett. However, many people with vertigo go undiagnosed for years, incorrectly believing their only choice is to live in this debilitating state.
The east Cork-based physiotherapist became aware of this fact when training in vestibular rehabilitation at Emory University, Atlanta, US, where vestibular rehab is part of general physiotherapy training. She now works in conjunction with the Vestibular Disorders Association of America, the Migraine Association of Ireland, and through GP group training to raise awareness of vestibular disorders among Irish GPs and the public.
Vestibular rehabilitation evidence-based medicine is now considered the most successful management approach for people with dizziness and balance associated with disorders of vestibular system, Barrett says.
“It’s never normal to be dizzy regardless of your age. The most important thing to realise is that vertigo or dizziness is not something you have to live with. However, only when an accurate diagnosis is implemented can the correct management programme for you be put in place,” says Barrett.
Causes
There are many causes of dizziness and vertigo, most of which are not associated with any serious condition. They include low blood sugar, low blood pressure, dehydration, inner ear disorders, medication side effects, heart problems and anxiety or stress.
The vestibular system includes the parts of the inner ear and brain that help control balance and eye movements. If this system is damaged by disease, ageing, or injury, vestibular disorders can result.
Barrett explains: “[Some] 35 per cent of adults aged 40 years and older experience vestibular symptoms at some point in their lives. Dizziness is one of the most common reasons people go to A&E. Vestibular disorders affect balance and often produce disabling symptoms that include vertigo, dizziness, balance problems and difficulty concentrating.
“These life-altering symptoms can deeply inhibit a person’s ability to perform basic day-to-day tasks, and are compounded by their invisibility to others, making it difficult to understand that a person with vestibular dysfunction is probably struggling to remain orientated and functional.”
One of the most common vestibular disorders is Benign Paroxysmal Positional Vertigo (BPPV) which is caused by tiny crystals of calcium (otoconia) becoming displaced and floating around the ear canal. One of the most common symptoms of BPPV is vertigo, which is often accompanied by dizziness, imbalance and nausea. Symptoms can be brought on by a change in position such as turning over in bed, looking up, leaning forwards or bending down to pick something up.
Another common vestibular disorder is vestibular migraine which, unlike other forms of migraine, does not cause pain in many people. The predominant symptoms are vertigo, dizziness, loss of balance, disorientation, motion and light sensitivity, and visual distortion.
People with vestibular migraine often undergo a multitude of medical consultations and extensive lab, imaging and other diagnostic evaluations without any diagnosis, says Barrett.
“In addition, vestibular suppressant medications are often given, increasing postural instability and further compounding the situation. Without a diagnosis, but with persisting symptoms, patients become disillusioned and hopeless. Some patients are given a diagnosis of ‘vertigo’ which is in fact a symptom – not a disorder. That’s why many people with these symptoms can go undiagnosed for several years incorrectly thinking that their only choice is to live with it. Like any condition, accurate diagnosis is the essential starting point and so once these patients are diagnosed with vestibular migraine, they can then be successfully managed.”
Triggers
Many of Barrett’s vestibular migraine patients report a family history of migraine, but on some occasions there is only a family history of “vertigo” stemming from misdiagnosed vestibular migraine. The known migraine triggers such as certain foods and environmental, emotional and hormonal changes can also trigger vestibular migraine.
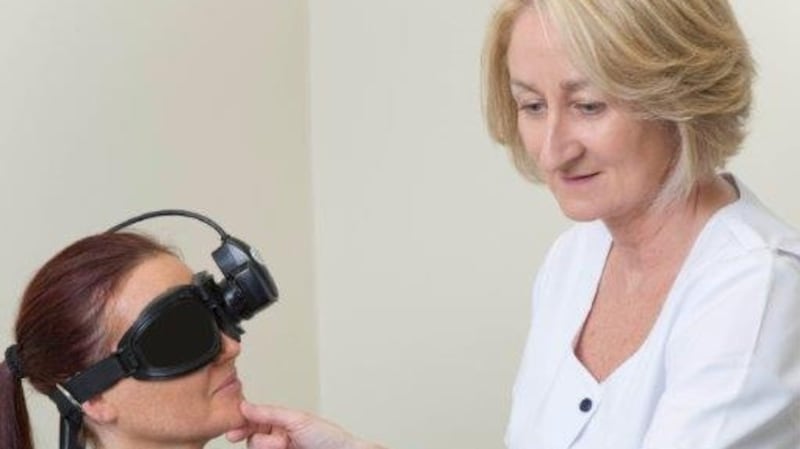
An accurate diagnosis for vestibular disorders is vital, says Barrett. A detailed medical history and physical exam followed by functional vestibular testing using infra-red goggles can identify the root cause of the problem. Once an accurate diagnosis is identified, appropriate treatment can begin which may include vestibular rehabilitation therapy (VRT), medication, surgery or elimination of a provoking drug.
Vestibular rehabilitation therapy includes a manoeuvre that eliminates BPPV by moving the displaced calcium particles out of the affected inner ear canal. It’s a hugely successful treatment, according to Barrett, with 95 per cent of people symptom-free following one manoeuvre and the other 5 per cent after a repeated manoeuvre. A programme of vestibular rehab exercises which train people to focus and move their head at the same time is also prescribed to be performed at home.
Head movements
Many people with vestibular disorders avoid moving their head because it causes them to feel dizzy and nauseous, but this avoidance of head movements further compounds the condition, explains Barrett. She has to train people to move their heads despite the short-term dizziness so they can get better and back to their normal lives.
A physiotherapist for 30 years, Barrett has always loved her work but she is hugely passionate about vestibular rehab which now forms the bulk of her workload as people come from all over the country for treatment.
“It makes such a difference to people’s lives, it helps them get their lives back and is incredibly rewarding work to be involved in.”
She is keen to share her training and expertise in diagnosing and treating vestibular disorders with more Irish GPs so people are not forced to suffer unnecessarily while undiagnosed.
“When a patient is diagnosed with ‘vertigo’ by their GP, they are usually put on vestibular suppressants. People on medical cards with no access to an ENT consultant often stay on this medication for years which further suppresses the vestibular system and hinders function. This can greatly limit a person’s lifestyle, lead to low mood and force them to time take off or give up work when all that is needed is to identify the cause of their vertigo and treat it appropriately.”
Pádraig Carroll: vestibular migraine
Teacher Pádraig Carroll had been suffering from dizziness for a few years on and off, but put his symptoms down to blood pressure issues. However, his condition deteriorated last year after he was hit with two infections and he was left with severe dizziness, balance problems, nausea and fatigue.
The Kilkenny man was diagnosed with vertigo by his GP and referred to a consultant geriatrician who sent him for an MRI, which was clear. He was prescribed medication, but saw no major improvement in his symptoms.
“By late October, I was totally debilitated. I felt like I had a permanent hangover, constant nausea and a muzziness in my head. I didn’t have sharp pain, more of a general discomfort and I was constantly fatigued. There was no question of me being able to work, it really put me under.”
Carroll had never heard the word vestibular until he met Sheila Barrett at East Cork Physiotherapy, Balance and Acupuncture Clinic and she diagnosed him with vestibular migraine.
As well as a rehab exercise programme, Carroll came off his medication (after consultation with his doctor) and went on a standard migraine diet which involved cutting out caffeine, chocolate, citrus fruits, alcohol and other foods.
“I noticed an immediate improvement when I started doing the exercises and diet. I’m still not 100 per cent better, but I was able to get back to work in January and am improving a bit every week. I have to avoid triggers like stress, infections and certain foods, but I am back walking every day again which is a great form of stress relief.”
Margaret Downey: BPPV
When Margaret Downey (77) started experiencing problems with her balance that caused her to “trip over nothing” on a number of occasions, she told nobody as she felt it was just a normal part of ageing.
“My balance wasn’t right, I was leaning to the left when I walked and I was extremely tired all the time. When I start something, I always finish it to the bitter end but I was leaving things unfinished and that was bothering me because it’s not my style. I fell a few times but made no fuss about it. I just thought everybody falls as they get older, but I know now it’s not normal.”
Living near the sea in Castletownbere, Downey had swam in the sea all her life but started to have difficulties swimming due to her lack of co-ordination and had to stop.
It wasn’t until early January of this year that the great grandmother finally sought help when things got even worse.
“One morning, as I got out of bed everything tumbled backwards. It was a terrible sensation, like being in an airplane somersaulting backwards. It was very frightening as I didn’t know what was happening. I gradually got up and was okay as the day went on, but I started to get a floating sensation when I turned on my right side in bed. I was also having problems with my sight, it was as if there was broken glass at the side of the lens of my glasses when there was nothing wrong with them.”
She went to the GP who told her she had vertigo and prescribed medication. The following week, she went to see vestibular physiotherapist Sheila Barrett in east Cork who diagnosed benign paroxysmal positional vertigo (BPPV), a condition where tiny particles called otoconia become dislodged in the inner ear and move around in the wrong place.
The physiotherapist was able to identify which of the three inner ear canals was affected by observing Downey’s eye movements using special infra-red goggles. She used a manoeuvre to move the displaced particles out of the affected panel back to where they should be and gave Downey a series of exercises to do at home to promote full recovery.
“As soon as I sat up after that treatment, I felt well again and the fear was gone. It had been getting worse and I had a fear of everything. Fear is a horrible thing, it takes away your confidence and I’m not that type of person. I couldn’t drive and even at Mass, I would be looking around to see if anybody I knew was near in case I needed help. Things hadn’t been right for a long time but thank God, I am 100 per cent back to myself again. I have my strength back, I’m not tired all the time and I’m sleeping better so my days are better. I would urge anybody with symptoms like mine to get help.”










